Imagine waking up after surgery with a titanium jawbone that fits you so perfectly it feels like it was always there — because, in a very real sense, it was designed just for you. That’s not science fiction anymore. In 2026, precision 3D printing has moved well past the prototype stage and into hospital operating rooms across the globe, quietly rewriting what’s possible in reconstructive and restorative medicine.
A few years ago, the idea of printing a patient-specific spinal cage or a customized hip socket overnight seemed like the kind of thing you’d read about in a tech magazine and forget. Now, orthopedic surgeons in Seoul, Berlin, and Houston are requesting these prints the same way they’d order a custom surgical tray. So let’s actually dig into what’s happening — with real numbers, real cases, and a clear-eyed look at where the limitations still lie.
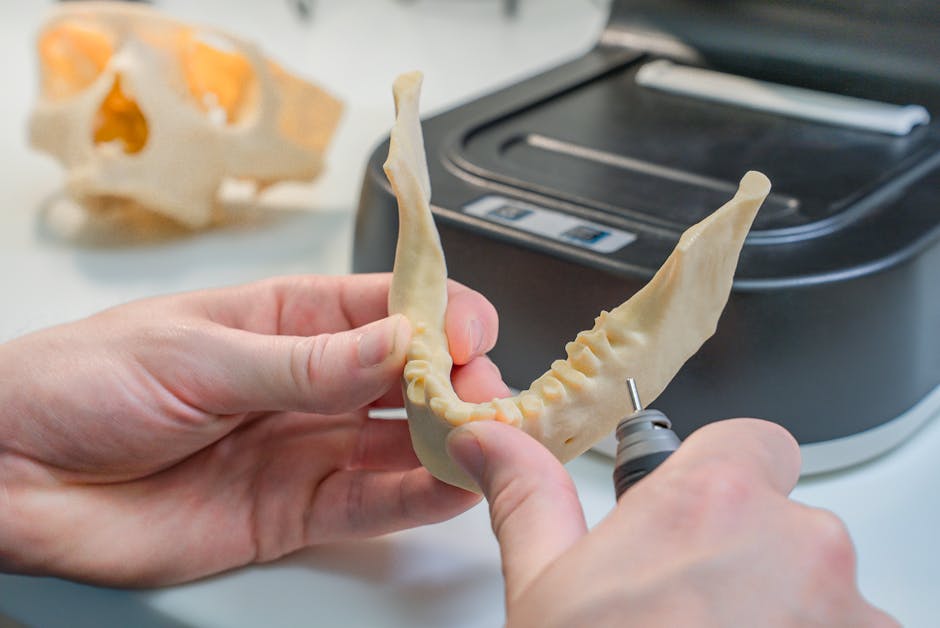
Why Precision Matters More Than You Think
Standard off-the-shelf implants work on the principle of “close enough” — a range of sizes that covers the statistical majority of patients. For most people, that’s fine. But for patients with unusual anatomy, trauma-related bone loss, or congenital conditions, “close enough” can mean the difference between full recovery and chronic pain.
Precision 3D printing — technically called additive manufacturing (AM) in biomedical contexts — allows implants to be fabricated from a patient’s own CT or MRI scan data. The result is a device that mirrors the patient’s unique geometry down to fractions of a millimeter. Here’s why that’s transformative:
- Reduced surgical time: When an implant fits perfectly, surgeons spend less time adjusting and more time closing. Studies published in early 2026 in the Journal of Orthopaedic Research show average surgical time reductions of 18–27% for custom 3D-printed hip and knee components compared to standard implants.
- Better osseointegration: That’s the process where bone actually grows into the implant. Lattice-structured titanium surfaces, only possible through 3D printing, increase surface area and mimic the trabecular (spongy) structure of natural bone, dramatically improving bonding rates.
- Lower revision rates: Early 2026 data from the Australian Orthopaedic Registry indicates a 14% lower 5-year revision rate for custom-printed implants versus conventional ones in complex pelvic reconstruction cases.
- Reduced inventory burden: Hospitals don’t need to stock dozens of implant sizes. A digital design file plus a certified printer replaces a warehouse shelf.
- Shorter patient recovery windows: Better fit generally means less micromotion at the implant site, which translates to faster and more stable healing.
The Materials That Make It Possible
Not every material can go inside a human body, so the material science here is just as important as the printing technology itself. Right now, the three dominant materials in biomedical 3D printing are:
- Titanium alloy (Ti-6Al-4V): The gold standard for load-bearing implants — think spinal cages, hip cups, and cranial plates. It’s biocompatible, lightweight, and incredibly strong.
- PEEK (Polyether ether ketone): A high-performance polymer used primarily in spinal and craniofacial applications. Its stiffness can be tuned to more closely match bone than metal, reducing stress shielding.
- Bioactive ceramics (like hydroxyapatite): Often used as coatings or in composite structures to actively encourage bone growth. Research groups at ETH Zürich and Yonsei University are working on fully printable ceramic scaffolds as of 2026.
Real-World Cases That Tell the Story
Numbers are useful, but cases make it real. Let’s look at a few examples from across the world that illustrate just how far this technology has come.
Case 1 — South Korea (Seoul National University Hospital, 2025–2026): A 34-year-old patient with aggressive osteosarcoma (bone cancer) in the pelvis underwent hemipelvectomy — the removal of half the pelvis. Traditionally, this procedure results in extreme functional limitation. Surgeons used a patient-specific titanium pelvic implant, 3D printed by the hospital’s in-house certified AM unit, in collaboration with a local biotech firm. The patient regained walking ability within 6 months, a timeline previously considered optimistic even under ideal conditions.
Case 2 — Germany (Charité – Universitätsmedizin Berlin): In early 2026, Charité published outcomes for a series of 22 patients who received custom-printed titanium cranial implants following traumatic brain injuries. The traditional approach uses manually molded PMMA (acrylic). The 3D-printed group showed a 31% reduction in post-operative infection rates and significantly higher patient-reported satisfaction scores related to cosmetic outcome — a factor that genuinely impacts psychological recovery.
Case 3 — United States (Mayo Clinic, Rochester): Mayo Clinic’s orthopedic division has been pioneering what they call “next-day implant” workflows — where a patient’s scan data is processed, the implant is printed and sterilized, and surgery happens within 36 hours of imaging. By Q1 2026, they’ve completed over 400 procedures using this workflow, primarily for acetabular (hip socket) reconstruction in revision surgeries where the original implant failed.
Where Are the Bottlenecks?
It wouldn’t be an honest conversation if we didn’t talk about friction points. Despite the excitement, there are real structural barriers to widespread adoption:
- Regulatory lag: The FDA, CE marking bodies in Europe, and MFDS in South Korea all have rigorous approval processes for custom implants. Each new design technically requires individual review, creating significant administrative overhead. Regulatory sandboxes and expedited pathways exist, but they’re not universal.
- Cost: A custom-printed titanium implant can cost 3–5x more upfront than a standard implant. Insurance reimbursement frameworks haven’t fully caught up with the technology, meaning cost often falls on hospitals or patients in non-covered cases.
- Printer certification and quality control: Not all 3D printers are equal. A poorly calibrated machine can produce micro-voids in metal that only show up under failure conditions inside the body. ISO 13485 certification for medical AM processes is increasingly required but not yet universal.
- Surgeon learning curve: Custom implants sometimes require modified surgical approaches. Training and workflow adaptation take time.
Realistic Alternatives — Who Should Consider What?
Here’s where I want to be genuinely helpful rather than just enthusiastic. 3D-printed custom implants are not the right answer for every patient or every hospital system. Let’s think through this together:
If you’re a patient facing a straightforward primary hip or knee replacement with normal anatomy and good bone stock — a high-quality standard implant from an established manufacturer (Stryker, Zimmer Biomet, Smith+Nephew) will very likely serve you excellently at lower cost and with a faster supply chain.
If you’re dealing with complex revision surgery, tumor resection, or congenital anomalies — this is where the custom 3D-printed route genuinely earns its premium. The functional and quality-of-life upside is demonstrably larger for these patient populations.
If you’re a hospital administrator in a resource-limited setting — consider hybrid models: partnering with third-party certified AM bureaus rather than investing in in-house printing infrastructure. Several companies in 2026, including 3D Systems’ healthcare division and Materialise, offer on-demand custom implant services with regulatory documentation included.
If you’re a healthcare policy maker — the data increasingly supports building reimbursement frameworks that differentiate “medically necessary custom” implants from elective customization. That distinction would unlock access for the patients who need it most without creating open-ended cost exposure.
The technology is genuinely remarkable, and the cases we’ve walked through show that lives are being meaningfully changed. But the path to broader impact runs through pragmatic problem-solving — regulatory clarity, smart reimbursement, and honest patient selection — not just better printers.
Editor’s Comment : What strikes me most about precision 3D printing in medicine isn’t the technology itself — it’s the philosophical shift it represents. For the first time, we’re seriously asking, “Why should the patient adapt to the implant?” and answering with “They don’t have to.” That’s a quiet revolution. But revolutions need infrastructure, and right now the gap between what’s technically possible and what’s systematically accessible is still wide. Keep an eye on how regulatory bodies in 2026 and beyond handle the classification of AI-assisted custom implant design — that’s the next pressure point, and honestly, it’s a fascinating one.
태그: [‘3D printed medical implants’, ‘precision additive manufacturing healthcare’, ‘custom titanium implants 2026’, ‘biomedical 3D printing cases’, ‘patient-specific implants surgery’, ‘orthopedic 3D printing technology’, ‘osseointegration implant innovation’]
Leave a Reply