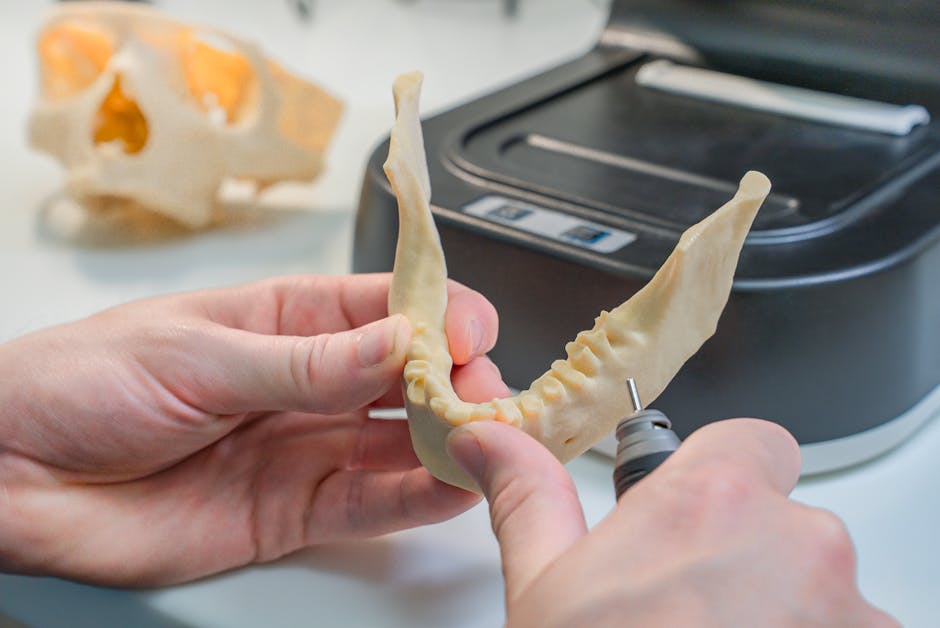
A colleague of mine — a biomedical engineer working at a Seoul-based orthopedic startup — told me something over coffee last month that genuinely stopped me mid-sip. One of their patients, a 14-year-old with a rare craniofacial bone defect, had received a titanium skull implant that was designed, printed, and sterilized in under 72 hours. The surgeon said it fit like a puzzle piece on the first attempt. No manual grinding, no intraoperative adjustments, no second-guessing. Just… perfect anatomical fit. That conversation sent me down a deep rabbit hole into the world of custom 3D-printed medical implants — and what I found is both technically fascinating and genuinely transformative for patients worldwide.
What Exactly Is a Custom 3D-Printed Medical Implant?
Let’s make sure we’re on the same page before we go deeper. Traditional implants — think hip prosthetics or spinal cages — are manufactured in standard sizes (small, medium, large) and surgeons essentially pick the closest fit. It works reasonably well, but “close enough” in surgery has real consequences: micro-movement, stress shielding, early implant failure, or just chronic discomfort.
Custom 3D-printed implants flip this entirely. Here’s the typical workflow:
- Step 1 – Imaging: Patient undergoes high-resolution CT or MRI scanning (sub-millimeter slice thickness, often 0.3–0.5 mm)
- Step 2 – Segmentation & CAD Modeling: Software like Materialise Mimics or 3D Slicer converts DICOM data into a precise 3D anatomical model; engineers then design the implant geometry around it
- Step 3 – Material Selection: Titanium alloy (Ti-6Al-4V ELI), PEEK (polyether ether ketone), bioceramic composites, or patient-specific bioresorbable polymers
- Step 4 – Printing: Selective Laser Melting (SLM) or Electron Beam Melting (EBM) for metals; FDM or SLA for polymer scaffolds
- Step 5 – Post-processing: Heat treatment, surface finishing, passivation, sterilization (gamma irradiation or ethylene oxide)
- Step 6 – Regulatory Clearance & Delivery: Device-specific 510(k) or PMA pathway in the US; CE marking in Europe; MFDS approval in South Korea
The Numbers Don’t Lie: Market Growth Is Explosive
Here’s where the data gets genuinely exciting. According to industry analysis compiled through early 2026, the global 3D-printed medical implant market was valued at approximately $2.3 billion USD in 2024 and is projected to reach $6.8 billion by 2030 — a compound annual growth rate (CAGR) of around 19.7%. That’s not hype; that’s infrastructure-level investment.
Breaking it down by segment:
- Orthopedic implants (spinal cages, hip cups, knee components): ~42% of market share
- Craniomaxillofacial (CMF) implants: ~21% — fastest growing due to trauma and tumor reconstruction cases
- Dental implants & guides: ~18% — heavily driven by consumer-facing digital dentistry
- Cardiovascular scaffolds: ~11% — still largely in clinical trial phase
- Other (ear, joint, spine navigation tools): ~8%
The key driver? Improved osseointegration. Studies published in journals like Acta Biomaterialia and Biomaterials consistently show that porous lattice structures achievable only through additive manufacturing — with pore sizes between 300–600 micrometers — dramatically outperform traditional smooth-surface implants in bone ingrowth and long-term fixation strength.
Real-World Case Studies: Who’s Actually Doing This?
This is where it gets grounded and real. Let me walk you through some standout examples from both domestic Korean and global contexts:
Zimmer Biomet (USA) — Their “Persona IQ” smart knee system now incorporates patient-specific instrumentation (PSI) guides printed from CT data, reducing surgical time by an average of 22 minutes per procedure. Their additive manufacturing facility in Warsaw, Indiana, runs 24/7 metal powder bed fusion systems. (Reference: zimmerbiometinstitute.com)
Materialise NV (Belgium) — Perhaps the most prolific software-to-hardware pipeline in the space. Their SurgiCase platform has been used in over 100,000 planning cases globally. In partnership with hospitals like UZ Leuven, they’ve produced patient-specific mandible plates for oral cancer reconstruction that reduced revision surgery rates by an estimated 34%.
Meditec (South Korea) — Operating under MFDS (Ministry of Food and Drug Safety) regulatory framework, this Seoul-based company has produced over 3,000 custom CMF implants since 2020, primarily for post-trauma facial reconstruction. Their turnaround time from scan to sterile implant has been reduced to under 5 business days as of 2026.
EOS GmbH (Germany) — The EOS M 290 and M 400 systems are the de facto gold standard in metal SLM for medical-grade parts. Their titanium powder specification (Ti-6Al-4V ELI per ASTM F3001) is what most FDA-cleared metal implant manufacturers are running.

The Technical Challenges Nobody Talks About (But Should)
Okay, here’s where I channel some real engineering frustration — because this technology isn’t without its headaches. Having worked adjacent to biomedical device development pipelines, let me share what actually slows things down:
Residual stress and warping — In SLM printing, the rapid heating and cooling cycles create internal stresses in metal parts. For a femoral stem with complex geometry, you can get up to 15–20% dimensional deviation at thin-wall sections without proper thermal simulation and support strategy. Post-build stress relief annealing (typically 800–900°C for titanium) is non-negotiable, but adds cost and lead time.
Powder contamination — Medical-grade titanium powder has a strict particle size distribution (15–45 μm for fine feature resolution). Even minor moisture contamination or cross-contamination with other alloys can compromise mechanical properties. ISO 13485-certified facilities run humidity-controlled powder rooms with laser diffraction particle analysis — this infrastructure is expensive.
Regulatory timelines — A custom implant under the FDA’s custom device exemption (21 CFR 812.3(b)) can sometimes bypass traditional 510(k), but the documentation burden is substantial. In Europe, the EU MDR (2017/745), fully enforced since 2021, significantly tightened notified body scrutiny on additively manufactured devices. Expect 18–36 months for full market authorization on novel implant designs.
Where Is This All Heading in 2026 and Beyond?
A few trends I’m watching closely right now:
- Bioprinting integration: Companies like Organovo and Korean startup T&R Biofab are pushing toward hybrid implants — a 3D-printed titanium scaffold seeded with the patient’s own osteogenic cells. Clinical trials are ongoing in 2026 for load-bearing bone applications.
- AI-driven design optimization: Generative design tools (Autodesk Fusion, nTopology) are now integrated with AI that automatically optimizes lattice topology for specific patient bone density maps pulled from CT Hounsfield unit values. This used to take weeks; now it takes hours.
- Point-of-care printing: Major hospital systems in Singapore, Germany, and South Korea are investing in in-house metal printing facilities to cut the supply chain entirely. Samsung Medical Center in Seoul has announced plans to operationalize an in-house SLM unit by late 2026.
- Bioresorbable implants: PLLA and PCL-based scaffolds that dissolve over 12–24 months as bone regrows are moving through clinical validation rapidly — particularly exciting for pediatric patients who otherwise face revision surgery as they grow.
Realistic Considerations for Patients and Clinicians
If you’re a patient researching this for a personal decision, or a clinician evaluating whether to refer a case for custom implant consideration, here’s what to realistically weigh:
- Cost: A custom titanium CMF plate might run $3,000–$12,000 USD more than a stock implant; insurance coverage varies significantly by jurisdiction and clinical justification
- Lead time: Even in 2026, 5–15 business days is realistic for most custom metal implants — emergency cases need a contingency plan
- Not always superior: For straightforward hip replacements in normally-proportioned adults, standard implants from proven designs still have multi-decade clinical outcome data. Custom isn’t always better — it’s about matching the right tool to the right problem
- Surgeon experience matters: The best implant design still depends on surgical execution; seek centers with documented experience in patient-specific device implantation
The most important takeaway? Custom 3D-printed implants aren’t a gimmick or a luxury upgrade — for complex anatomies, revision cases, pediatric reconstructions, and tumor resections, they represent a genuine paradigm shift in surgical precision. But they’re also not a universal replacement for proven standard-of-care devices. The future is clearly hybrid: data-driven patient matching that determines when customization delivers measurable clinical benefit versus when a well-designed stock implant does the job just as well.
Editor’s Comment : If I had to point someone toward a starting resource right now, I’d direct clinicians to Materialise Medical and the FDA’s 3D Printing in Medical Devices guidance page — both are surprisingly accessible and kept current. For patients, the most empowering question you can ask your surgeon isn’t “Can I get a 3D-printed implant?” but rather “Is my anatomy a candidate for patient-specific design, and what outcome data exists for this approach?” That single question will tell you very quickly how sophisticated your clinical team’s thinking is on this topic.
📚 관련된 다른 글도 읽어 보세요
- 의료용 맞춤형 3D 프린팅 임플란트, 2026년 현재 어디까지 왔을까?
- Additive Manufacturing in Aerospace Components 2026: What’s Actually Changing on the Factory Floor
- Best DIY NAS Hardware Recommendations for 2026: Build Your Own Powerhouse Home Server
태그: 3D printed medical implants, custom implant technology, patient-specific implants, selective laser melting medical, orthopedic additive manufacturing, biomedical 3D printing 2026, titanium implant osseointegration
Leave a Reply